ICU Patient Monitoring and Tele-Critical Care in Rural America
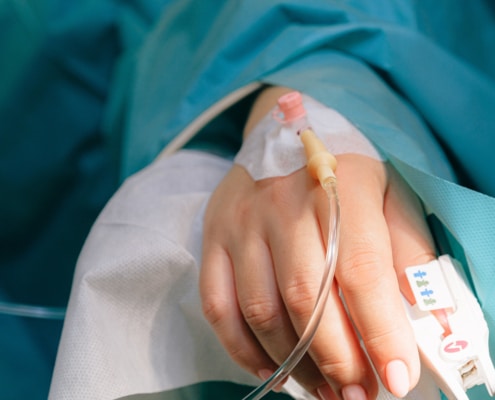 ICU Patient Monitoring Services For Remote and Rural Hospitals
ICU Patient Monitoring Services For Remote and Rural Hospitals
ICU patient monitoring is set to address ongoing labor shortages being felt by many remote and rural critical care facilities in America. As healthcare facilities continue to be burdened by a lack of skilled talent, ICU health monitoring systems offer access to specialized talent and human resources that have become in short supply in a post-pandemic world. Regardless of the distance, ICU patient monitoring has been born out of necessity and is one of the latest innovations in telehealth that can help healthcare facilities of all kinds address their needs and offer quality care to their patients. When remote and rural hospitals embrace ICU patient monitoring healthcare solutions, the difference can be life and death.
ICU care monitoring from Intercept Telehealth offers on-demand access to experienced, board-certified intensivists, specialists, and critical care nurses at any hour of the day. When rural hospitals enlist ICU patient monitoring telehealth systems, your facility can provide specialized patient care that would otherwise be unavailable. Ensure your facility can provide quality care for all patients and embrace innovation as a means of providing the quality care that every patient deserves.
ICU Patient Monitoring: Five Benefits For Rural Hospitals
Address the complexities of skilled labor shortages in rural healthcare systems and explore the top benefits of utilizing ICU health monitoring systems for your hospital.
1. Exceptional Patient Satisfaction
When a healthcare facility is properly equipped with ICU patient monitoring systems it keeps them close to home with the healthcare team members that they are familiar with. Many rural hospitals still have primary care physicians who directly admit to an open ICU, and ICU patient monitoring allows these team members to tap into specialized labor, without ever physically bringing them to the remote job site. In turn, this helps patients gain access to exceptional care, without having to transport them to another facility entirely.
2. Decrease in Hospital Transfers
For rural hospitals who refer patients to tertiary medical center, a reduction in hospital transfers allows providers to “load balance” their ICUs across the system, while increasing average patient census and surgical/procedural volumes.
Excessive hospital transfers are stressful for patients, but also costly to rural healthcare facilities. A reduction in hospital transfers means an increase in reimbursement; by increasing medically appropriate hospital days and professional charges to cash-strapped rural hospitals that are under unprecedented financial pressure.
Keeping patients close to home means not just a decrease in transfers, but also an increase in a hospital’s Medicare Case Mix Index and Medicare/Medicaid reimbursement rates. This provides hospital systems with greater leverage when negotiating with private third-party payor negotiations.
3. Increase Staff Retention With Improved Recruitment
Rural ICUs may not have the patient census to justify a full-time intensivist on staff. Tele-ICU offerings from Intercept allow rural systems to use hospitalists, internists, and even family practitioners to staff their ICUs, without them ever visiting the physical workplace.
When hospitals experience a lack of clinical expertise, it can lead to staff burnout, and turnover of registered nurses, respiratory therapists, and physicians, complicating ongoing labor shortages for the hospital itself. Tele-ICU systems help mitigate these challenges, helping hospitals build workforces that have access to the support they need to conduct their work to the best of their abilities.
4. Adherence to ICU Best Practices
Tele-critical care brings tertiary and quaternary ICU organizational culture and best practices to rural and remote healthcare settings. With the use of standardized care algorithms, checklists, and order sets, rural hospitals can streamline their productivity, and create standardization in their work practices while seeing a decrease in CLABSIs, CAUTIs, and VAEs/VAPs.
5. Improved ICU Triage
Tele-ICU expertise allows for early identification of patients on the medical floor, rural ICU, or rural ED settings who should be transferred immediately. With increased efficiency and access to skilled human resources, a rural hospital will see an immediate increase in ICU Triage efficiency helping patients get the care they need with reduced wait times. Make sound decisions that are in the best interest of the patient and ensure they receive the highest quality care available to them.
ICU Patient Monitoring Offered By Intercept Telehealth
Intercept Telehealth is a Telehealth care provider, founded and led by physicians who are well aware of the challenges facing rural hospitals across the United States. Every patient deserves quality care. By leveraging state-of-the-art technology and data analytics, hospitals and healthcare facilities anywhere in the world can access critical care specialists regardless of physical boundaries. Now, even the most remote hospitals can provide the gold standard of quality care, improve efficiency, and improve the quality of life of patients and entire workforces.
Contact Intercept Telehealth today to learn more about the technology designed to support rural and remote healthcare facilities, both big and small, anywhere in the world.
References
Goedken CC, Moeckli J, Cram PM, Reisinger HS. Introduction of Tele-ICU in rural hospitals: Changing organisational culture to harness benefits. Intensive Crit Care Nurs. 2017 Jun;40:51-56. doi: 10.1016/j.iccn.2016.10.001. Epub 2017 Feb 16. PMID: 28216177.
McLeroy RD, Ingersoll J, Nielsen P, Pamplin J. Implementation of Tele-Critical Care at General Leonard Wood Army Community Hospital. Mil Med. 2020 Feb 13;185(1-2):e191-e196. doi: 10.1093/milmed/usz147. PMID: 31247104.
Harris GH, Baldisseri MR, Reynolds BR, Orsino AS, Sackrowitz R, Bishop JM. Design for Implementation of a System-Level ICU Pandemic Surge Staffing Plan. Crit Care Explor. 2020 Jun 15;2(6):e0136. doi: 10.1097/CCE.0000000000000136. PMID: 32695999; PMCID: PMC7314315.